
Onchocerciasis is a disease caused by the invasion of the organism by threadlike worms called filaria belonging to the species Onchocerca volvulus. Its gravity is due to the fact that it very frequently gives rise to blindness in populations living on the banks of rivers, whence its name "river blindness". It rages especially in Africa but also in Central America and in a little breeding ground in Yemen, regions into which the disease has been introduced by groups of slaves since the fifteenth century.
Its causes, its clinical manifestations and modes of transmission have only been determined lately. The Colonial Health Service has played a great part in these discoveries, in particular in the study of the endemic in Africa and when the disease has been eradicated.
The means used against its spread and the advent of a very efficacious medicine, facilitate the controlling of the disease, "relieving humanity of this incapacitating disease".
ONCHOCERCA VOLVULUS
At the time of the great quest for infectious agents in 1892, a German missionary in Ghana takes out subcutaneous nodules from patients and finds worms in them. A naturalist identifies them as filaria bearing the name of Onchocerca volvulus. These worms of variable length, depending on their sex (5 cm for males and 50 cm for females), live under the skin, freely or encysted, for a period of about twelve years. Their eggs, in the uterus of the female, engender microscopic larvae, call microfilaria, which are to be found abundantly in the dermis of the skin, the lymphatic ganglions and the eye tissues. They are microfilaria that live for one or two years and are responsible for skin and eye troubles.
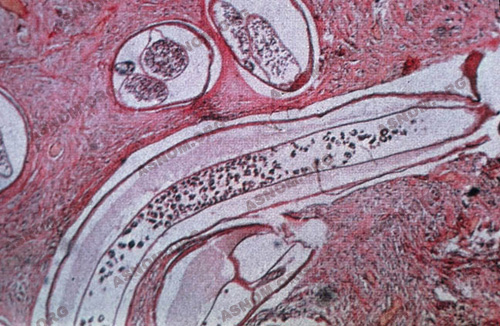
CLINICAL MANIFESTATIONS
The disparate signs of this disease are only gradually attributed to a single cause.
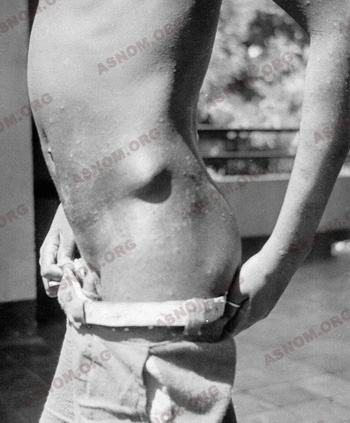
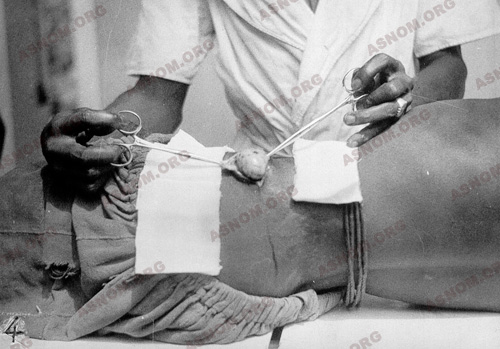
The most striking clinical manifestation is the presence, under the skin, of nodules the size of a mandarin, causing no pain, hard, rolling easily over the bones underneath : the hips, the ribs. They never suppurate and end up by being calcified. As early as 1902, the physicians of the Colonial Health Service report the existence of these nodules in the inhabitants of Oubangui-Chari. Then Brumpt finds them in the Congo. The Germans too observe them in the populations of Cameroon.
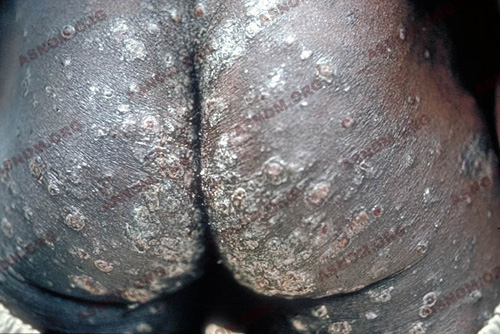
Another precocious and constant symptom in the skin : an intense pruritus which evolves in stages and provokes lesions due to scratching ; the skin thickens, then it atrophies and loses colour, taking on the aspect of a lizard skin. The most frequently affected zones are the lower portion of the trunk and the lower limbs. Ouzilleau*, observing the concomitance of lesions in the skin with subcutaneous nodules, names this thickening of the dermis "volvulose cutanée".
In 1920, two dermatologists in Algiers, Montpellier and Lacroix, studying a form of scabies observed in infantrymen from West Africa, discover microfilaria of Onchocerca volvulus in the dermis. They call it "scabies of filaria" ("gale filarienne"). Ouzilleau*, Laigret* and Lefrou* report the same phenomenon in Brazzaville in 1921. The cutaneous lesions are manifestly of the allergic type, the proteins of the microfilaria sensitizing the dermic tissues. The lesions due to scratching are a gateway for the entrance of microbes which aggravate the clinical situation.
Another locality that may be affected has been observed : the abiotrophy of the ganglions of the groin may lead to a thickening of the skin which concerns the derma and hypoderma, Elephantiasis. It is to be observed most frequently in the lower limbs and the genitals. The deformation consists of fleshy folds separated by fissures, the breeding ground of all superinfections, which can sometimes become monstrous, causing great functional disorders. The huge development of the genital organs in cases of Elephantiasis has sometimes been attributed to Onchocerca Volvulus. In 1913, Ouzilleau* is convinced that this filaria could be responsible for the disease because he finds it in all the Elephantiasis patients. This is confirmed by the Belgians, Rodhain and Dubois. Laigret*, on the occasion of a census permitting evaluation in Sudan, is more reserved. However, if among the filaria responsible for the onset of the malady, Onchocerca Volvulus may play a role, the cause by far the most frequent of Elephantiasis is Lymphatic Filariasis.
The role of Onchocerciasis in the development of eye troubles was recognized at a late date, in 1919, by Roblès and Pacheco-Luna in Guatemala. In Africa, where the rate of blindness is higher than in America, the ocular symptoms are noted but the possible causes are so numerous that the relationship with dermic nodules is not taken into consideration. Syphilis is blamed by Cloitre* in Madagascar, whereas it is ruled out by Bertrand* in Togo. Others think the trouble may stem from trypanosomiasis and especially an undesirable effect of treatment with arsenicals. Lefrou* and Goarnisson incriminate Avitaminosis A. And it is only in 1932 that a Belgian ophthalmologist, Hissette, perfectly identifies the eye lesions caused by Onchocerciasis, in the Belgian Congo. Many other works follow with, in particular after the creation of the IOTA, the studies of Colonial Health Service ophthalmologists : D’Haussy*, Monjusiau*, Vedy*. All the eye tissues can be affected : the cornea, the iris, the ciliary body, the membrane of the retina and the optic nerve.
THE MODE OF TRANSMISSION
The intervention of a mosquito having been established in the transmission of Malaria, Ouzilleau*, in 1913 in the Congo, blames a mosquito of the genus Culex for the spread of Onchocerciasis. A few years later, the Belgians Rodhain and Van den Braden suspect mosquitoes of the genus Stegomyia and bugs. Roblès in Guatemala finds the culprit in another species in 1919. His observations lead him to conclude that the transmitting agent is a stinging and sucking insect which has a predilection for the temples and the neck. There is only one such insect in the region under study : the female simulium, a genus of little black flies two millimetres in length.
Blacklock in 1924 in Sierra Leone confirms the conclusions arrived at by Roblès and clarifies the evolution of the microfilaria in the infected simulium : in the course of eight days, the microfilaria pass from the digestive tube into the thoracic muscles and then reach the proboscis, whence they escape at the moment of stinging. His work will be confirmed in 1946.
Unlike the American simulium, that of Africa has a tendency to sting the legs. In Africa, these little flies are to be found in swarms during the day. Their stings are painful and bloody. They are capable of flying long distances, tens of kilometres. The simulium lay eggs on plants and rocks amidst troubled running waters that are strongly oxygenated. In a few days, they can colonise a whole river. The eggs are stuck together in packets by a viscous substance. Before turning into flies, the larvae live in the stream of water.
THE STUDY OF THE ENDEMIC IN AFRICA
Onchocerciasis is a disease that is exclusively rural. It is, together with Trachoma, one of the great causes of blindness and attacks millions of people in the world. It is estimated that, in intertropical Africa alone, it affects more than a million persons and causes blindness in a hundred thousand among them.
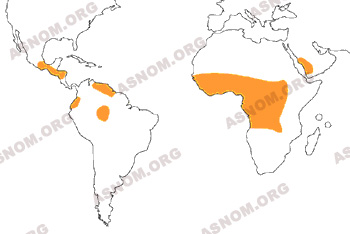
Until the beginning of the 1930s, the Sudan-Sahelian regions are not included among the zones where the propagation of Onchocerciasis is recognized, in spite of the detection of a breeding ground in Sudan by Lecomte* in 1915. In fact no methodical investigation was undertaken. Richet* is the first to make an epidemiological examination of patients suffering from Elephantiasis, carriers of nodules and having problems of vision in Upper Volta in 1938.
At the same time, Muraz*, Director of the SGAMS, instructs his research groups to detect cases of Onchocerciasis. They are to be found everywhere : in French West Africa (AOF), and in Togo. Up to that time, recruiting commissions had enlisted carriers of cutaneous nodules, considering that it was not incompatible with military status. From 1938, Richet* opposes such recruitments in order to wipe out the spread of the endemic.
Unfortunately, from 1942 onwards, a section of the personnel go to the fronts, vehicles and fuel are requisitioned and the search for people afflicted with the disease is halted.
After the war, in 1947, Onchocerciasis being considered a great endemic, the fight against it is taken up again with the extensive means available to the SGHMP. Rouzic* gives Puyuelo* the task of making an inventory of Onchocerciasis in Upper Volta. The first figures obtained in 1948-1949 indicate the gravity of the infection : among 102 188 subjects examined, 17 188 are carriers of nodules, 8 094 of them have eye problems of varying seriousness and 1 838 are blind. The rates of infection and eye troubles are 5 or 6 times higher in the neighbourhood of the Volta. "The proximity of the great rivers devours the eyes" is a popular saying in Mossi country which is irrigated by the three Voltas (Black, White and Red). In fact, taking samples of serous fluid systematically by means of the scarification of the skin enables the estimation of the rate of infection in regions around waterways to be 20 %. Pfister* observes that half of those who are carriers of Onchocera volvulus microfilaria in the skin have not got nodules. Mere palpation of the skin therefore reveals only one half of the cases subject to infection.
Jonchère*, who has just replaced Le Rouizic* as the Director of the SGHMP in 1953, organizes systematic investigations at the level of the Federation. They end at the beginning of the year 1954 and help to estimate the extension of the ravages in French West Africa (AOF). The number of those afflicted with Onchocerciasis in the AOF is estimated to be 200 000, one half of the cases being in Upper Volta where, among nearly a million persons examined, 46 000 cases of Onchocerciasis are found. This figure (which proves to be inferior to the actual number of sufferers) at last gives a measure of the importance of the endemic, for its occurrences are capricious and the causes of blindness are numerous in these climates. An examination by an ophthalmologist is necessary in order to pin down with certainty Onchocerciasis as the cause.

The creation by Labusquière* of a "Mobile ophthalmologic group in Upper Volta" with Monjusiau*, Rolland* and De Gabvriel* renders possible therapeutic practices and, above all, precise epidemiological, ophthalmologic and parasitological studies. Picq* perfects a method of counting microfilaria which makes possible a quantitative approach to the degree of infection. Rolland* demonstrates that serious eyesight complications and blindness (up to 10 % in the villages that are most affected) are limited to the inhabitants who live closest to the river banks, there where contact with simulium is intense and protracted.
These researches lead to the identification of Onchocerciasis patients who risk eyesight problems, those who need to be treated urgently. Thanks to the action of this section of the SGHMP, Upper Volta becomes, in 1966, the first African country where the inventory of Onchocerciasis subjects is complete. This will be a determining element later on in the choice of the country where the large-scale campaign for prevention by disinsectisation will be initiated.
THE MEANS OF COMBAT
For a long time, after having demarcated the zone of the disease and detected thousands of patients, the colonial physician remains helpless before Onchocerciasis because he disposes of no really effective remedy. The traditional African solution is to move the village twenty or thirty kilometres from the river into places that are drier, less fertile but less dangerous.
The systematic ablation of cysts undertaken in Guatemala from 1915 did not show any lasting improvements, for re-infection usually follows. In Africa too the results are disappointing.
In 1947 Hewit uses a derivative of piperazine, diéthylcarbamazine ou notézine, which is active against other filaria. Puyuelo*, in 1949, obtains good results in the case of 70 Onchocerciasis patients but the medicine is badly tolerated by the organism (severe pruritus and eye complications). He observes violent reactions of the allergic type due to the brutal destruction of microfilaria. Moreover, notézine has no effect on adult filaria.
Suramin, which is used to combat Sleeping Sickness, is somewhat efficacious against adult worms. But it is a dangerous product, sometimes fatal, difficult to administer and inefficacious in the case of those in areas where the disease is endemic, and where infections are recurrent.
Faced with these failures, medical treatment is orientated towards the protection of healthy subjects by the destruction of the vectors, the simulium. It is understood that the combat will be long because the work of interrupting transmission must last longer than the life span of the adult worm, about at least 14 years. An attempt in Kenya, in an isolated breeding ground, succeeds in eradicating the vector and stopping transmission.
Richet*, in the 1950s, undertakes a campaign of spreading insecticides using helicopters in a region of Chad. But this attempt is rapidly brought to an end because the breeding ground is rapidly re-infested by neighbourhood rivers that have not been treated.

From 1955, M. Ovazza, an entomologist in the office of French overseas scientific research (ORSTOM) arrives in Bobo Dioulasso, at the Muraz Centre, to study the biology of black flies and to advocate methods of combat. At the same time, Richet* succeeds Masseguin* as Director of the SGHMP and decides to create a new Onchocerciasis section. Quélennec* starts assessing the effect of several larvicides (temephos among others), upon simulid larvaes, and perfects an original method for measuring the resistance of larvaes to pesticides. This method will be used by WHO. The Parasitology section of the Muraz Centre (Lamontellerie*, Picq*), the ophthalmologists of the IOTA (Veilleux*, Le Breton-Oliveau*) and the mobile team in Upper Volta work in close collaboration with the entomologists of Bobo-Dioulasso, helped by Le Berre and Philippon. From 1959 on, sufficient funds are allotted, and important means are used to fight the disease like the helicopter spraying of all the rivers and canals of an area with a larvicide of the temephos type.
After the independences, OCCGE in West Aftrica and OCEAC in Central Africa take over from SGHMP. In 1975, a large scope action is undertaken, but two years prior to that, the mission of Assistance to governments (PAG Mission) is created. It is headed by Hamon. Its objective is to establish a plan of action, the budget, and the economical and social windfalls of the fight against onchocerciasis. WHO, supported by the World Bank, FAO, PNUD and donations from numerous donor nations, initiates the Onchocerciasis Control Programme (OCP). Ziegler, director of the programme is installed in Ouagadougou, and in Geneva, Quélennec* takes on the responsability of a support agency. The choice of the land of operation is dictated by the perfect knowledge of the endemic, thanks to the work of the SGHMP. Nowhere else is the "inventory of fixtures" as accurate in what concerns Onchocerciasis. Over a territory one and a half times that of France, with its centre in Upper Volta, regular spraying is started again several times each month. Ten million inhabitants are in the area. The programme lasts twenty years and costs 120 million dollars. The spread of Onchocerciasis is halted.
The simulium vector is not eradicated but it is controlled. All the indications of Onchocerciasis infection diminish progressively in spite of the absence of any medical treatment. The international program ends in 2002. It is known that, after this date, epidemiological surveillance will have to remain vigilant in order to prevent the resurgence of tiny residual seats of infection likely to become starting points of new bursts of Onchocerciasis.
An other aspect of the fight against onchocerciasis is chemioprophylaxy. In the early 1980s, a tremendous progress was made when ivermectine (approved in 1987) was launched under the name of mectizan. It is well tolerated by patients. Taking a tablet once every six months destroys the microfilaria and inhibits the egg-laying of adult filaria. Its use from 1980, together with the campaign against disease carriers (vectors), gives hope that, with the support of international solidarity, this epidemic could one day disappear altogether from intertropical Africa.
In front of the main entrance of the WHO Headquarters in Geneva, a commemorative statue has been erected. On the base of the monument there is a plaque that tells passers-by :
This distressing depiction of a child guiding an adult who has lost his sight after having contracted the river blindness, a plague that afflicts poor communities. "At the end of the track" was a common sight in wide areas, and most particularly in Africa.
By uniting their efforts in an outstanding partnership, the onchoceriasis control programme in West Africa, the African program of fight against onchoceriasis and the eradication programme of onchoceriasis in the Americas have relieved humanity of this incapacitating disease, thus contributing to reduce poverty.

This statue testify to the succes of a unic action for public health which also has contributed to the socio-economical development.
On October 6 1999, on the occasion of the 25th anniversary of the programme of fight against onchocerciasis in West Africa, the statue was inaugurated by Dr Gro Harlem Brundtland, general director of WHO.
On the bronze, the list of the donors who helped finance the cost of the statue, follows.
For further information :
– Comité d’experts de l’onchocercose. Edit. Genève. Série de rapports techniques. 1966,335,101p.
– OMS : Epidémiologie de l’onchocercose. Série de rapports techniques. Edit. Genève. 1976,597,108p.
– Vedy J. Graveline J. : Onchocercose in Précis d’ophtalmologie tropicale. Diffusion de librairie. Edit. Marseille 1979,267,152-167.
– Picq J.J. Philippon B. : Onchocercose Encycl. Méd.-Chir. Maladies infectieuses 8-112 A50, 10-1981.
– OMS/OCP : 10 ans de lutte contre l’onchocercose OCP Ouagadougou Edit. 1985 183p.

